 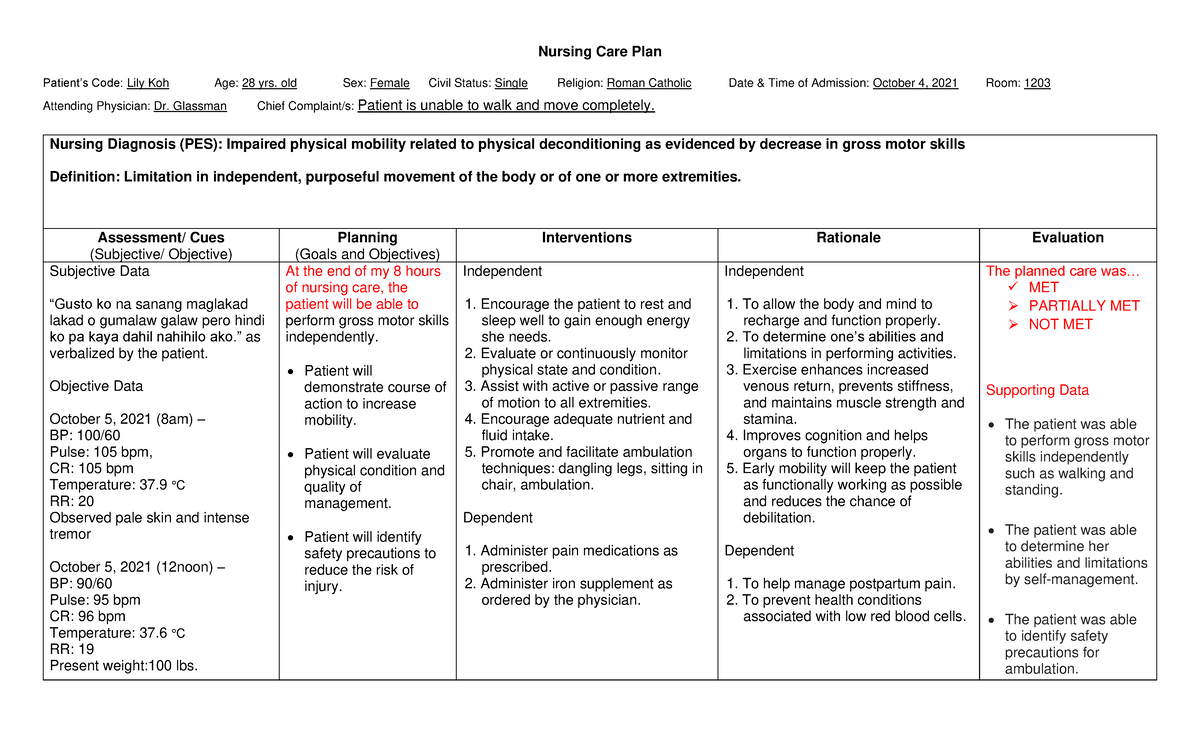 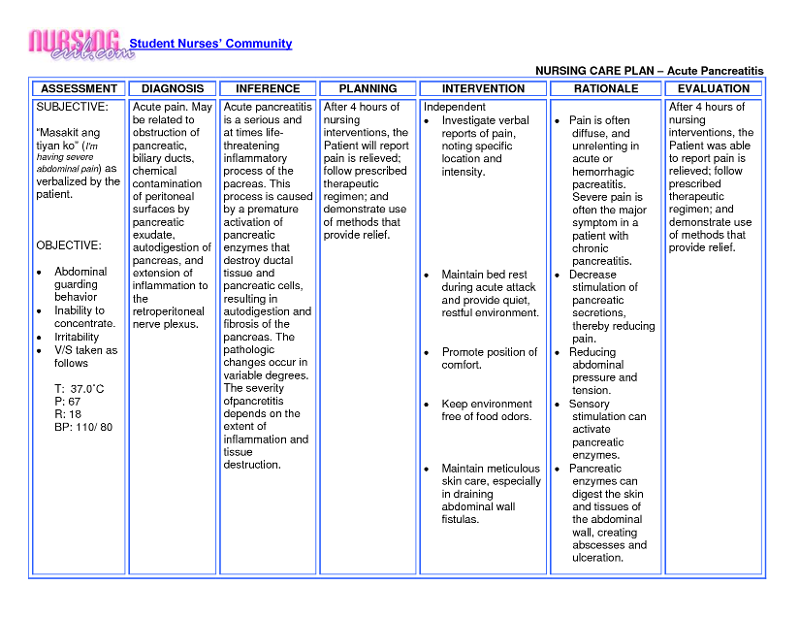 
Perform hourly rounding to check on the patient’s needs and prevent falls. įor bed-bound patients, elevate the head of the bed to 30 to 45 degrees, unless medically contraindicated, and turn and reposition the patient every two hours. Monitor oxygenation levels and provide supplemental oxygen as prescribed to maintain adequate oxygenation, especially during ambulation. , įor patients at risk for developing pneumonia due to immobility, encourage adequate fluid intake to liquefy pulmonary secretions, and teach deep breathing and coughing exercises to prevent atelectasis. Educate the patient about appropriately using assistive devices and other fall precautions. Administer medications if warranted and consider nonpharmacologic measures such as repositioning, splinting, and heat/cold application to reduce musculoskeletal discomfort. Monitor the patient’s level of pain by using a valid pain intensity rating scale. Be aware that pain and fear of falling can be major deterrents to a patient’s willingness to ambulate or perform physical therapy. Encourage or perform active or passive range of motion exercises as prescribed by the physical therapist. See details about early mobilization protocols earlier in this chapter.Įncourage the patient to perform activities of daily living (ADLs) as independently as possible and participate in prescribed physical therapy. For example, a patient undergoing a cardiac catheterization may be mobilized within a few hours following the procedure, whereas a patient undergoing total knee arthroplasty may begin mobilizing 24 hours following the surgery. Mobilization efforts, ranging from dangling on the edge of the bed, sitting up in a chair, and assisting with early ambulation, depend on the patient’s unique circumstances, such as their medical condition and surgery performed. To avoid or minimize complications of immobility, mobilize the patient as soon as possible and to the fullest extent possible. Nursing interventions promote a patient’s mobility and prevent effects of immobility. The American Academy of Nursing issued a recommendation in 2014 stating, “Don’t let older adults lie in bed or only get up to a chair during their hospital stay.” This recommendation highlights the importance of implementing evidence-based measures to promote activity during hospitalization to prevent functional decline in older adults. Hospitalization poses a risk for altered functional status of older adults due to acute illness, decreased mobility, and the negative effects of bedrest. Conditions such as osteoarthritis, orthostatic hypotension, inner ear dysfunction, osteoporosis resulting in hip fractures, stroke, and Parkinson’s disease are among the most common causes of immobility in old age. Older adults are at increased risk for immobility. As teenagers become adults, the nurse provides education about the effects of alcohol and other drugs on balance and safety while driving. When working with school-age children, nurses provide education to prevent injury that can occur with activity, such as using helmets and knee pads to prevent injury while bicycling and skateboarding. Parents are educated about these developmental milestones during well-child visits. For example, infants move their limbs, hold their head up, roll, sit, crawl, stand, and then eventually walk. Īt each stage of growth and development, the nurse assesses a patient’s mobility and provides appropriate education. Note if urinary incontinence is occurring due to the inability of the patient to reach the restroom in time. Monitor 24-hour trend of intake and output, as well as for symptoms of dysuria, urgency, or frequency. Assess for the presence of urinary tract abnormalities related to immobility, such as suprapubic distention or tenderness that can result from urinary retention. If constipation is suspected, palpate the patient’s left lower quadrant for signs of stool presence. Ask the patient about the date of their last bowel movement, and monitor stool patterns and stool characteristics. 
Assess for potential signs of atelectasis and pneumonia.Īssess the gastrointestinal system by inspecting for distension, auscultating bowel sounds, and palpating the abdomen for tenderness. Assess for the presence of lower extremity edema and for signs of a potential deep vein thrombosis (DVT).Īssess the respiratory system, including respiratory rate, oxygen saturation, lung sounds, chest wall movement and symmetry, and depth and effort of respirations. Assess the cardiovascular system, including blood pressure, heart sounds, apical and peripheral pulses, and capillary refill time. Read more details about performing a “ Musculoskeletal Assessment” chapter in Open RN Nursing Skills.īecause immobility can negatively affect several body systems, perform a thorough assessment for patients with impaired mobility. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
